Key Takeaways
- Acupuncture is WHO-recognized for stroke rehabilitation — the World Health Organization lists stroke and its sequelae among the conditions for which acupuncture has been proved effective through controlled trials
- Scalp acupuncture produces rapid neurological changes — developed in China in the 1970s, this technique stimulates motor, sensory, and speech cortex areas through the scalp, with fMRI studies confirming real-time activation of damaged brain regions
- Clinical evidence is substantial — a Cochrane review of 31 trials (4,257 patients) concluded that acupuncture combined with standard rehabilitation improves neurological deficit scores, motor function, and daily living ability
- China integrates TCM into standard stroke care — most major Chinese hospitals have integrated TCM-Western medicine stroke units, giving patients access to both conventional neurology and acupuncture/herbal medicine from day one
- Treatment window matters — earlier TCM intervention (within the first 3 months post-stroke) correlates with significantly better outcomes, though improvements are possible even years later
The Rehabilitation Gap After Stroke
Every year, approximately 15 million people worldwide suffer a stroke. Of those who survive, roughly 60% are left with some form of lasting disability — motor impairment, speech difficulties, cognitive changes, spasticity, depression, or chronic pain.
Conventional stroke rehabilitation — physical therapy, occupational therapy, speech therapy — is effective, but progress often plateaus after the first 3–6 months. Many stroke survivors reach a point where their therapists tell them: "This is as good as it's going to get."
This is where the Chinese medical system diverges from Western practice. In China, TCM has been integrated into acute and post-acute stroke care for decades. The approach is not alternative — it is complementary. Chinese neurologists and TCM practitioners work together in integrated stroke units, combining:
- Conventional thrombolysis and neurosurgery (acute phase)
- Standard physical, occupational, and speech therapy
- Acupuncture — body, scalp, and electroacupuncture
- Chinese herbal medicine — for brain protection, circulation, and recovery
- Tuina therapeutic massage — for spasticity and range of motion
The question is no longer whether TCM can help stroke recovery. The question is how much additional benefit it provides, and for which patients.
How Acupuncture Works for Stroke Recovery: The Mechanisms
Neuroplasticity Enhancement
The brain's ability to reorganize itself — neuroplasticity — is the foundation of all stroke recovery. Acupuncture has been shown to enhance neuroplasticity through several documented mechanisms:
Neurotrophic factor upregulation: Acupuncture stimulation increases expression of brain-derived neurotrophic factor (BDNF), nerve growth factor (NGF), and glial cell line-derived neurotrophic factor (GDNF). These proteins are essential for neuronal survival, axonal growth, and synapse formation in the penumbral region surrounding the stroke lesion (Li et al., 2020, Neural Regeneration Research).
Synaptogenesis and dendritic remodeling: Animal studies using controlled cortical impact models show that electroacupuncture at GV20 (Baihui) and GV14 (Dazhui) increases synaptophysin expression and dendritic spine density in the peri-infarct cortex — directly measurable structural brain repair.
Mirror neuron system activation: fMRI studies demonstrate that acupuncture at motor points (LI4, LI11, ST36) activates both ipsilateral and contralateral motor cortex, suggesting it can recruit compensatory neural pathways in the undamaged hemisphere.
Cerebral Blood Flow Improvement
Stroke recovery depends heavily on adequate blood supply to the damaged and surrounding brain tissue. Transcranial Doppler studies have shown that acupuncture increases cerebral blood flow velocity in the middle cerebral artery by 10–20% — particularly when applied to points along the Governing Vessel (Du meridian) on the scalp and neck (Litscher et al., 2004, Neurological Research).
Anti-Inflammatory and Neuroprotective Effects
Post-stroke neuroinflammation causes secondary brain damage that can continue for weeks after the initial event. Acupuncture has been shown to:
- Reduce microglial activation and pro-inflammatory cytokines (TNF-alpha, IL-1beta, IL-6) in the ischemic penumbra
- Decrease blood-brain barrier permeability, reducing cerebral edema
- Inhibit neuronal apoptosis through upregulation of Bcl-2 and downregulation of Bax and caspase-3
- Reduce glutamate excitotoxicity — a major driver of secondary neuronal death
Spasticity Reduction
Post-stroke spasticity affects 20–40% of survivors and is a major barrier to functional recovery. Electroacupuncture has been shown to reduce spasticity through:
- Modulation of gamma motor neuron excitability
- Reduction of alpha motor neuron firing rates
- Increased reciprocal inhibition between agonist and antagonist muscles
- Changes in H-reflex parameters consistent with reduced spinal cord excitability
Scalp Acupuncture: China's Contribution to Neurological Treatment
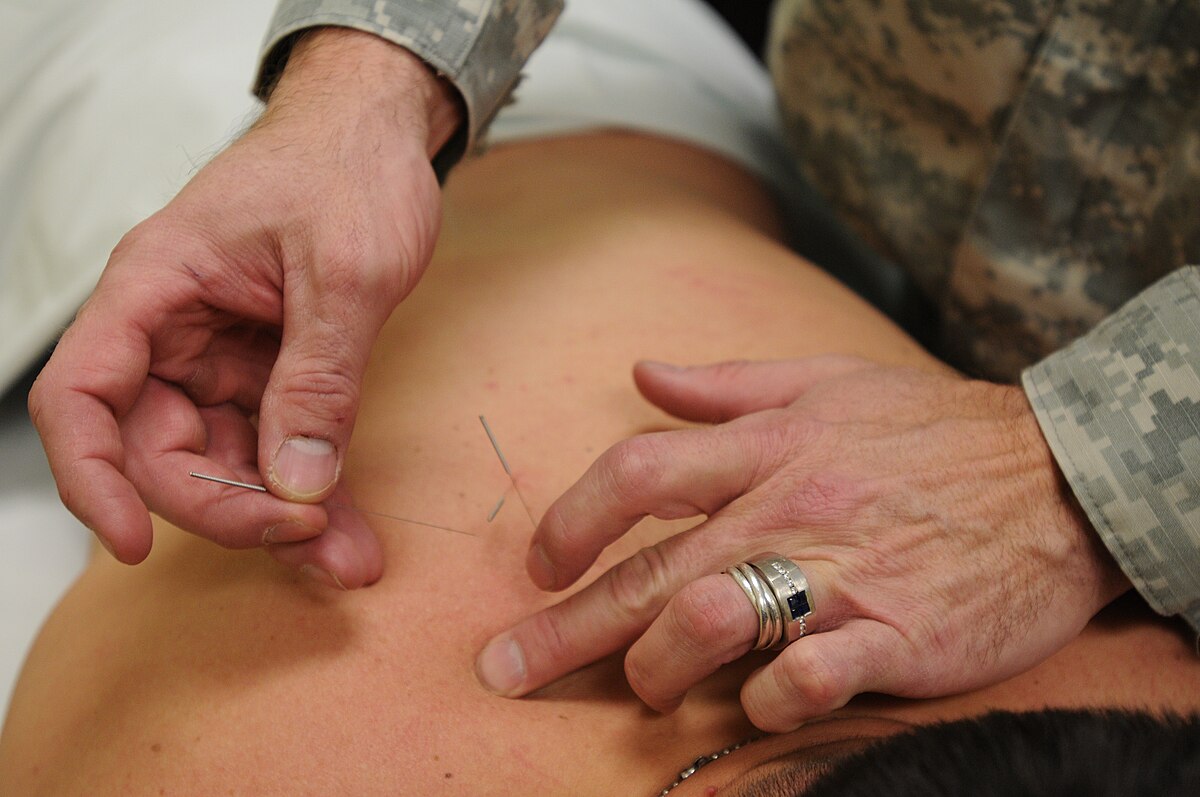
Scalp acupuncture (头针疗法) is perhaps the most important TCM innovation for neurological rehabilitation. Developed in the 1970s by Dr. Jiao Shunfa (焦顺发) and others, it maps conventional neuroanatomy onto the scalp surface — motor cortex, sensory cortex, speech areas, balance zones — and stimulates these areas through thin acupuncture needles.
How Scalp Acupuncture Differs from Body Acupuncture
| Feature | Body Acupuncture | Scalp Acupuncture |
|---|---|---|
| Theoretical basis | Meridian theory | Cortical neuroanatomy |
| Needle depth | Into muscle/fascia | Subgaleal (beneath scalp aponeurosis) |
| Key technique | De qi sensation | Rapid rotation (200+ rpm) |
| Active exercise | Optional | Critical — patient moves during stimulation |
| Onset | Gradual over sessions | Often immediate improvement during first session |
| Primary target | Systemic regulation | Direct cortical stimulation |
Scalp Acupuncture Zones and Their Applications
Motor zone (运动区): Runs along the anterior border of the central sulcus projection on the scalp. Divided into upper (leg), middle (arm), and lower (face/speech) segments.
- Upper 1/5: contralateral lower limb motor recovery
- Middle 2/5: contralateral upper limb motor recovery
- Lower 2/5: facial paralysis, speech (motor aphasia), dysphagia
Sensory zone (感觉区): Parallel to and behind the motor zone, corresponding to the postcentral gyrus.
- Used for: post-stroke numbness, paresthesia, central post-stroke pain
Speech zones:
- Speech zone 1 (语言一区): motor aphasia (anterior, Broca's area projection)
- Speech zone 2 (语言二区): sensory aphasia (posterior, Wernicke's area projection)
- Speech zone 3 (语言三区): nominal aphasia
Balance zone (平衡区): Over the cerebellar projection on the occiput.
- Used for: ataxia, balance disorders, dizziness
The Jiao Method in Practice
During a typical scalp acupuncture session for hemiplegia:
- Needles are inserted into the contralateral motor zone (opposite to the paralyzed side)
- The practitioner performs rapid rotation (200+ revolutions per minute) for 2–3 minutes
- While needles are being stimulated, the patient actively attempts to move the affected limb — this simultaneous stimulation and voluntary effort is critical to the technique's effectiveness
- Stimulation is repeated 2–3 times during a 30-minute session
- Between stimulation rounds, the patient continues rehabilitation exercises with needles retained
Many practitioners and patients report visible improvement in motor function during the first session — a phenomenon that, while sometimes temporary, demonstrates the technique's ability to activate dormant neural pathways.
Clinical Evidence for TCM in Stroke Recovery
Cochrane Reviews and Meta-Analyses
Cochrane Review (2006, updated 2016): Evaluated 31 RCTs with 4,257 stroke patients. Conclusion: acupuncture combined with standard stroke rehabilitation was associated with significant improvement in neurological deficit scores, motor function (Fugl-Meyer Assessment), and activities of daily living (Barthel Index) compared to rehabilitation alone. The review noted that study quality was variable but the overall direction of evidence was consistently positive (Wu et al., 2006, Cochrane Database of Systematic Reviews).
Updated meta-analysis (2022, Frontiers in Neurology): Pooled data from 82 RCTs involving 7,628 patients. Acupuncture as adjunctive therapy showed:
- Neurological deficit improvement: MD = -3.41 (95% CI: -4.52 to -2.30)
- Barthel Index improvement: MD = 8.67 (95% CI: 5.83 to 11.52)
- Fugl-Meyer motor score improvement: MD = 6.83 (95% CI: 4.29 to 9.37)
- Statistically significant benefits in both acute (<30 days) and subacute/chronic phases
Scalp Acupuncture-Specific Evidence
Motor Recovery: A multicenter RCT across six Chinese hospitals (n=362) compared scalp acupuncture + rehabilitation vs. rehabilitation alone in patients 2–12 weeks post-ischemic stroke. At 8 weeks:
- Fugl-Meyer upper extremity score: 42.3 vs. 34.8 (p<0.001)
- Action Research Arm Test: 38.7 vs. 29.4 (p<0.001)
- Functional Independence Measure: 95.2 vs. 82.6 (p<0.001)
Aphasia (Speech Recovery): A 2020 study in Acupuncture in Medicine evaluated scalp acupuncture (speech zones 1–3) combined with speech therapy in 120 post-stroke aphasia patients. At 12 weeks:
- Western Aphasia Battery score improvement: 28.4 points vs. 16.7 points (speech therapy alone)
- Naming ability sub-score showed the largest differential improvement
- fMRI confirmed increased activation in perilesional language areas
Dysphagia (Swallowing Difficulty): A systematic review of 18 RCTs (1,434 patients) found that acupuncture combined with swallowing rehabilitation improved standardized swallowing assessment scores significantly more than rehabilitation alone, with reduced pneumonia incidence — a critical complication of post-stroke dysphagia.
Chinese Herbal Medicine for Stroke
Bu Yang Huan Wu Tang (补阳还五汤) — "Tonify the Yang to Restore Five-Tenths" — is the most extensively studied Chinese herbal formula for stroke recovery. Originally described by Wang Qingren in 1830, it contains Huang Qi (astragalus) as the chief herb, with blood-moving herbs including Dang Gui, Chuan Xiong, Tao Ren, Hong Hua, Chi Shao, and Di Long (earthworm).
Pharmacological research shows this formula:
- Promotes angiogenesis in the ischemic penumbra
- Reduces blood viscosity and inhibits platelet aggregation
- Increases BDNF expression in the hippocampus and cortex
- Protects the blood-brain barrier
- Reduces neuronal apoptosis
A 2021 network meta-analysis of 64 RCTs comparing different Chinese herbal formulas for ischemic stroke recovery ranked Bu Yang Huan Wu Tang as having the strongest evidence for improving neurological deficit scores when used as an adjunct to standard care.
What Integrated Stroke Rehabilitation Looks Like in China
The Chinese Integrated Stroke Unit Model
China's major hospitals operate integrated stroke units where Western neurology and TCM work together — not as "alternative" vs. "conventional," but as a unified care team.
Typical Daily Schedule — Inpatient Stroke Rehabilitation:
| Time | Activity |
|---|---|
| 7:30 AM | Chinese herbal decoction (customized formula) |
| 8:00 AM | Physical therapy (conventional) |
| 9:30 AM | Scalp acupuncture with active exercise |
| 10:30 AM | Occupational therapy |
| 11:30 AM | Body acupuncture or electroacupuncture |
| 2:00 PM | Speech therapy (if indicated) |
| 3:00 PM | Tuina therapeutic massage for spasticity |
| 4:00 PM | Moxibustion or cupping (if indicated) |
| 7:00 PM | Evening herbal medicine |
Treatment Phases
Acute Phase (0–14 days):
- Focus: Brain protection, prevent secondary damage
- TCM role: Herbal formulas for clearing phlegm and opening orifices (e.g., An Gong Niu Huang Wan for consciousness disorders), acupuncture for early stimulation
- Note: TCM is adjunctive — thrombolysis, thrombectomy, and acute neurological management take priority
Subacute Phase (2 weeks – 3 months):
- Focus: Maximize neuroplasticity window, intensive rehabilitation
- TCM role: Scalp acupuncture 5×/week, body acupuncture daily, herbal medicine for circulation and qi recovery
- This is the critical treatment window — the brain is most receptive to reorganization
Chronic Phase (3 months – 2 years+):
- Focus: Continue functional gains, manage complications (spasticity, pain, depression)
- TCM role: Ongoing acupuncture 2–3×/week, herbal formula adjustment, manage post-stroke depression and insomnia
- Improvement is still possible in this phase but typically slower
Treatment Timeline Expectations
| Function | Initial Signs of Improvement | Meaningful Recovery | Maximum Expected Gain |
|---|---|---|---|
| Gross motor (walking) | 1–4 weeks | 2–4 months | 6–12 months |
| Fine motor (hand) | 2–6 weeks | 3–6 months | 12–18 months |
| Speech (aphasia) | 2–4 weeks | 3–6 months | 12–24 months |
| Swallowing | 1–3 weeks | 1–3 months | 6 months |
| Cognition | 4–8 weeks | 3–6 months | 12–24 months |
| Spasticity control | 1–2 weeks | 1–3 months | Ongoing management |
These are general timelines for patients receiving integrated TCM + conventional rehabilitation. Individual results depend on stroke type, location, severity, age, and overall health.
Where to Get Integrated Stroke Rehabilitation in China
Top Centers for TCM-Integrated Stroke Rehabilitation
Dongzhimen Hospital, Beijing University of Chinese Medicine (北京中医药大学东直门医院)
- Pioneered China's integrated stroke unit model
- National Clinical Research Center for TCM Stroke Treatment
- Known for: scalp acupuncture rehabilitation, Bu Yang Huan Wu Tang research
- International patient services available
Huashan Hospital, Fudan University, Shanghai (复旦大学附属华山医院)
- One of China's top neurology departments
- Rehabilitation medicine department integrates TCM and Western approaches
- Known for: post-stroke hand function recovery, spasticity management
- Strong research collaboration with international institutions
Tianjin University of TCM First Affiliated Hospital (天津中医药大学第一附属医院)
- Internationally recognized for scalp acupuncture research
- Professor Shi Xuemin's "Xing Nao Kai Qiao" (醒脑开窍) acupuncture method originated here — now used nationally
- Known for: consciousness disorders, post-stroke aphasia, advanced scalp acupuncture protocols
Cost Comparison
| Treatment Component | China (Integrated) | US (Rehab Facility) | Japan |
|---|---|---|---|
| Inpatient rehab (per day) | $80–200 | $1,500–3,000 | $300–800 |
| 30-day inpatient program | $2,500–6,000 | $45,000–90,000 | $9,000–24,000 |
| Acupuncture session | $15–40 | $75–150 | $30–80 |
| Scalp acupuncture (specialized) | $20–50 | Rarely available | $40–100 |
| 3-month intensive program | $6,000–15,000 | $100,000–250,000 | $25,000–60,000 |
Is TCM Stroke Rehabilitation Evidence-Based?
The honest answer: the evidence consistently supports acupuncture as a beneficial adjunct to standard stroke rehabilitation. The effect sizes are clinically meaningful — patients receiving integrated treatment recover more function, faster, than those receiving conventional rehabilitation alone.
Important caveats:
- TCM does not replace acute stroke treatment — clot-busting drugs and surgical intervention save lives and must come first
- The quality of individual studies varies, though the overall body of evidence across hundreds of trials points in the same direction
- Scalp acupuncture requires specialized training — not all acupuncturists are qualified
- Earlier treatment produces better results, but improvement is possible even in chronic stroke (>1 year)
For patients who have been told they have reached their recovery plateau, TCM offers a credible additional avenue worth exploring — particularly when delivered within China's integrated hospital system where both approaches work together.
How OriEast Helps Stroke Patients
Stroke rehabilitation in China requires careful coordination between neurology, TCM, rehabilitation medicine, and daily logistics for patients who may have significant physical limitations.
What we provide:
- Hospital and specialist matching — identifying the right integrated stroke unit based on your specific deficits (motor, speech, cognitive, swallowing)
- Pre-arrival assessment — reviewing imaging, discharge reports, and current functional status with your Chinese medical team
- Visa and travel coordination — including wheelchair-accessible transport and accommodation near your treatment hospital
- Daily medical accompaniment — bilingual support during rehabilitation sessions, acupuncture treatments, and doctor consultations
- Family communication — regular progress updates and video consultations for family members who cannot travel
- Discharge planning — coordinated transition including a home exercise program, herbal formula continuation plan, and remote follow-up schedule
Considering stroke rehabilitation in China? Contact OriEast for a free case review. We will assess your situation, recommend the most appropriate facility, and outline a realistic treatment plan and timeline.